
Charles R. Goulding and Andressa Bonafe have an engaging conversation with Mauricio Toro, co-founder and CEO of TECHFIT.
The combination of digital planning and 3D printing promises to considerably improve outcomes for patients while making surgeries more time and cost-effective. We had a conversation with TECHFIT’s co-founder and CEO Mauricio Toro, in which he gave us an overview of his company’s work along with his views on the challenges and opportunities of 3D printing in healthcare.
To start, could you tell us a little about yourself and the educational and professional experiences that ultimately led you to co-found TECHFIT?
I started as a motorsport engineer. My background is actually as an aerodynamicist for race cars. I worked with the Formula Three team in the UK. A family friend, who is my cofounder at TECHFIT, he’s a doctor and he introduced me to the medical field. He invited me to be a part of a medical device company and I pivoted my career towards the medical device space. When I got into the orthopedics field, I couldn’t help but compare it to the automotive industry. Race cars are a passion and a pinnacle of automotive innovation but they are not as critical to mankind as health. Even so, we were performing 3D simulations of the cars and 3D printing models for the wind tunnels. What I found was that this was not the case in the orthopedic field, which is very conservative. In most instances, doctors would walk into surgery with ten different sizes of implants and, akin to being in a shoe store, they would measure which implant would fit best (with the patient open). So it was clear to me that we now have the technology to make this better. And that’s how the whole idea of TECHFIT started.
Could you give us an overview of your company and its products? We’re especially interested to know how 3D printing plays into your offerings.
At TECHFIT we have developed an end-to-end platform for the creation of custom medical devices for orthopedics applications, such as bone and musculoskeletal reconstruction, neurosurgery, andcranio-maxillofacialand thoracic surgery. We’ve created a cloud-based software in which doctors can upload a CT scan and have it converted into a 3D model of the patient. This model can be used for virtual surgeries and collaboration with other doctors around the world to find the best treatment plan. We have surgical technicians and engineers available to help and make sure that whatever gets designed is manufacturable. So, in other words, we create a cloud-based environment where a case can be designed and followed up.
Once the design is done, we then proceed to print out anatomical models, surgical guides, and even implantable devices, using either our FDA-registered 3D printing capabilities or the client’s own. In this context, if a hospital plans to implement 3D surgical planning and 3D printing processes, we can help them through our partnership with Formlabs. We have fully validated the Formlabs printing equipment, so we can make sure that processes are up to medical standards. We take care of all the preventive maintenance, validation, and quality control.

What would you say are the most common areas of application for digital surgery planning so far and what would be some promising ones for the future?
For now, I would say that the biggest area, the early adopter, has been craniomasculofacial surgery. This is basically because the face is what we show the world. So there is a very high premium for accurate and precise reconstruction. I think what is coming next and it’s starting to get a lot of traction is joint replacement surgery, including shoulder, ankle, knee, and hip replacement. But for the future, what we see that is most interesting is that, with good software and 3D printers at the point of care, we can start doing trauma cases. So, for instance, imagine a patient that has been in a car accident and has a bone that is broken into many fragments. We can use rapid response 3D printing to make this patient’s recovery faster and to ensure that mobility is better than if we had used traditional methods.
On more of a general note, how do you see the role of 3D printing in the future of medicine?
I believe that the application of 3D printing in medicine is a process and that this process will have four stages. The first and most elementary stage is the printing of anatomical models to understand anatomy and for medical education purposes. I think this role has been pretty much fulfilled. We can improve the quality of the models, but this is the ground upon which everything is built. The next step, the second wave so to speak, is the 3D printing of medical devices. This kind of application is gaining traction because of all the supply chain challenges we saw due to COVID-19 and the complexity associated with manufacturing some of the devices we use now. The following step is 3D printing for bioactive substances, including scaffolds. There are now numerous startups with very interesting projects, such as 3D printing tricalcium phosphate for patient-specific scaffolds. Finally, the last step, which is the goal for all of us, is to 3D print tissue.
And what would you say are currently the most common challenges for healthcare practitioners to incorporate 3D printing and how to overcome them?
I believe there are basically three challenges and they are all interweaved. The first one is economical – there is a need to invest in a 3D printer, invest in talent, etc. This aspect is often discussed and there are undoubtedly a lot of hurdles to get past. I think, however, that there are other things hidden behind it. Rather than simply financial, it’s more of a talent problem. There is not a lot of knowledge about how to use 3D printing in a medical setting. So getting into medical 3D printing means you have to invest in a learning curve for someone. I believe this is one of the biggest barriers. Another one is reimbursement. If there isn’t a good quality framework or good quality talent, insurers will question the value of 3D printing and won’t pay for it. So I think we need to work to make it more cost-effective, which means dropping hardware costs and the cost of learning as an organization. We need to find creative ways to build around the costs of implementation and, once there is more widespread adoption, it’s going to be easier to prove the value of 3D printing and get players to reimburse it.
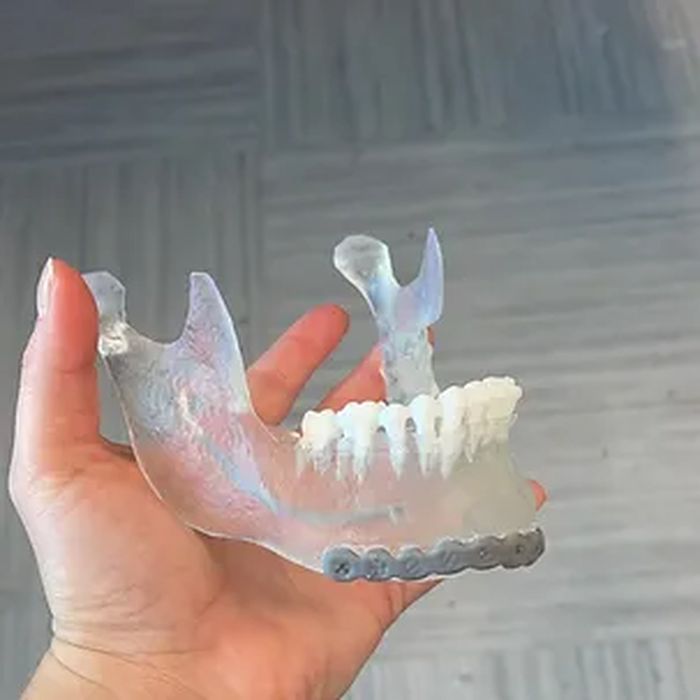
Going back to TECHFIT and its 3D printing applications, are there any other recent developments that are worth mentioning?
Yes, there are two important milestones that have happened recently. First, our software received FDA clearance. This is very important because it shows that we can do everything at a medical standard – not like a hobby 3D printing but medical grade 3D printing, which is what patients deserve. And, secondly, we have been working with the Mayo Clinic and one of their thoracic surgeons in Jacksonville, Dr. Matthew Thomas, to create new 3D-printed replacements for the chest. This would benefit patients that have infections from open heart surgery or tumors in their ribs. We just got a patent awarded for 3D-printed sternums made out of PEEK biomaterial. So we are very excited about that.
Conclusion
We were impressed with Mauricio Toro’s combination of technical and business knowledge and extensive experience. We were introduced to his work when researching our recently published Formlabs piece and examining one of their webinars. Mauricio’s technical expertise is self-evident and includes a recently issued patent. His business acumen is clear when he emphasizes the importance of developing practices that enable the reimbursement of 3D printing costs.
