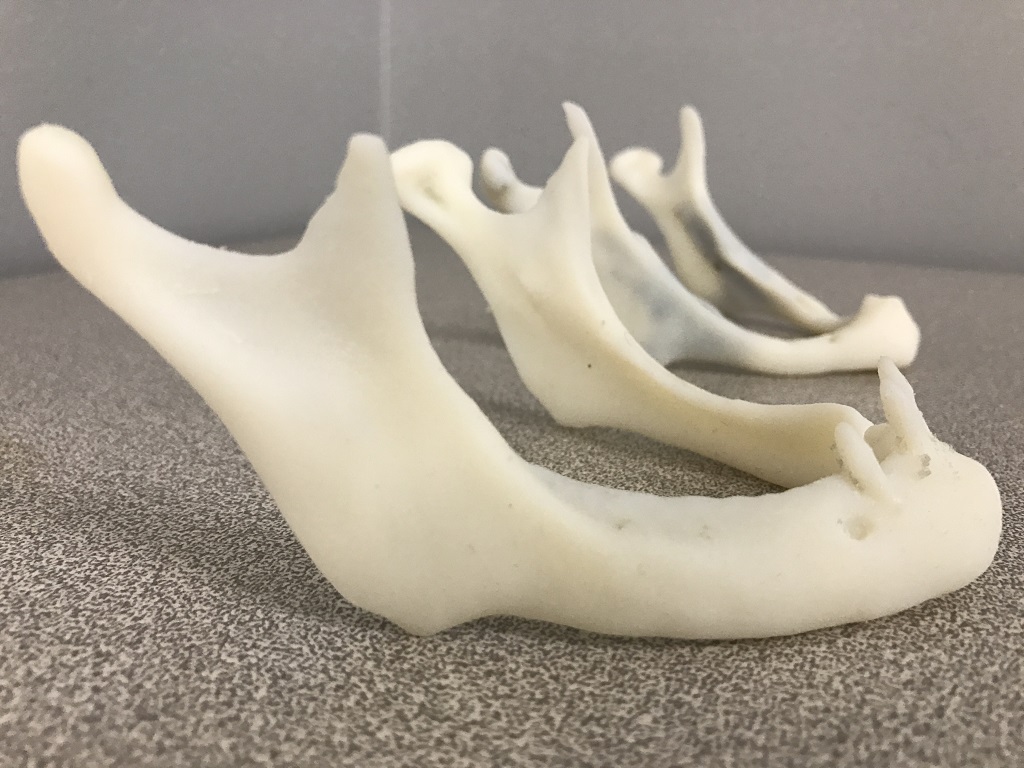
![3D printed mandibular model [Image via Stratasys]](https://fabbaloo.com/wp-content/uploads/2020/05/va_mandible_img_5eb09fd0b0702.jpg)
Closing out 2018 on a heartening note, I caught up with Stratasys and the VA on their cooperation to bring 3D printing and innovation into healthcare.
Michael Gaisford, Stratasys’ Director of Marketing for Healthcare Solutions, and Dr. Beth Ripley, the Chair of the VHA 3D Printing Advisory Committee at Veterans Administration (VA), share a look into mandibular reconstruction.
“The back history is that 3D printing has become a very important aspect of what we’re doing with our innovations within the VA hospitals. We really do have a really nice history of innovation and I think moving forward we are really trying to push the envelope on what innovation within the VA looks like, and 3D printing is a huge part of that,” Dr. Ripley explained as we spoke.
Gaisford noted in our chat that Stratasys has a deep engagement with the VA that has been going on for some time.
“We have a formal agreement with the VA to support their 3D printing program, and have provided printers and materials,” he said. “It’s created a seed for the VA that Beth Ripley has taken and run with, to drive much deeper energy and excitement around 3D printing and is turning it into a national model for distributed 3D printing across a national health network. The program is much larger than this one story, which highlights what Beth is doing with our CSR network.”
That CSR network — Corporate Social Responsibility — is responsible for seeing Stratasys’ 3D printing portfolio not just put to good use, but some of the best uses the technology sees. Actual human good.
The last time we spoke with Gaisford, the conversation focused on advanced prosthetic solutions. This time, mandibular surgery took center stage.
This is the story of a jaw. Of a lot of jaws.
Here we focus on Stratasys’ tech-driven role in bringing 3D printing to bear in mandibular surgery; in part two, Dr. Ripley shares the VA perspective.
The need for mandibular surgery — jaw reconstruction — can trace back to any number of health issues. Among the most common reasons are trauma, where an accident affects the jaw, or a tumor that either destroys or whose removal destroys a part of a jaw.
“The greater the damage and destruction, the more challenging the reconstruction is. There’s off-the-shelf products that can be used for this surgery but a jaw isn’t one-size-fits all, and surgeons end up having to shape the hardware. Doing that freehand in the middle of surgery, with the patient on the table under anesthesia, with people waiting around, is very stressful,” Gaisford explained, setting the scene.
By 3D printing the patient’s jaw, the surgical team can get hands-on with the exact anatomy they’ll be working with before entering the operating room. Mandibular implants generally come in three sizes: small, medium, and large. Not only selecting the best fit but shaping it appropriately for the specific patient ahead of time cuts both guesswork and operating time.
“One great technique is mirroring,” Gaisford continued, getting into applications for the technology. “Say the left side was damaged and needs reconstruction, and the right side is healthy. You can take the scan and CT data and mirror it, then print the healthy jaw and use it as a template. The team can bend the plate and choose the hardware according to that ideal jaw they’re trying to achieve after the surgery. They’ve pre-bent the plate, taken it to sterilization, and it goes into the operating team with them.”
This pre-OR work adds up — so much so that 80-100 minutes can be taken out of surgical time.
“With operating room time costing $80/minute, savings can be very substantial by reducing time. The shorter the time spent on the table, the better the recovery will be, with fewer anesthesia-related side effects, for example. It frees up surgical staff as well, so they have more time for more patients,” Gaisford continued.
Describing the clear-cut benefits of this use case as “one of those applications where there’s a clear win for 3D printing,” he added that Stratasys was excited to see the VA continue to work with the technology for their patient base around the country.
Various 3D printers are brought to bear in these applications, with both FDM and PolyJet technologies seeing use within the VA system. FDM models allow for a hands-on understanding and appreciation of anatomy at a relatively lower cost, while high-resolution, high-accuracy PolyJet prints can offer full color that, for instance, highlights blood vessels and other more detailed information. Gaisford noted that a wide variety of materials and machines are used in this application space, and the VA’s installed base of Stratasys technologies allows for choice in each case.
Just last month, Stratasys announced an important partnership with Materialise that leads to FDA-cleared 3D printed medical models made with its PolyJet technology. The clearance includes specific indications for use: cardiovascular, orthopedic, and craniomaxillofacial. Mandibular reconstruction falls under the last of these. The FDA clearance is a strong statement for point-of-care 3D printing such as that being embraced at the VA.
“I think this is one of those applications where 3D printing should be standard of care. Every mandibular reconstruction in the US, in the world, should be using a 3D printed model to save surgery time and money,” Gaisford said. “To me, this is one of those that’s a no-brainer.”
As medical 3D printing continues to be explored, more applications are being adopted as standards of care. Uses are flourishing in hospital labs to create patient-specific medical models, tools, cutting guides, and more.
“Every surgeon I talk to who’s used 3D printing sees the benefit, sees the value, and says so clearly this is how we should be treating our patients going forward,” Gaisford said in closing.
“We’re seeing 3D printing moving from being investigational research to identifying where it can play a role in standard of care.”
Read part two here.
Via Stratasys and VA Puget Sound Health Care System




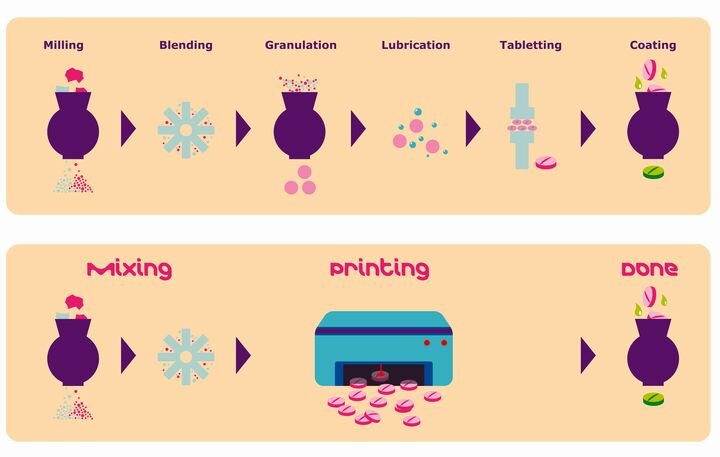




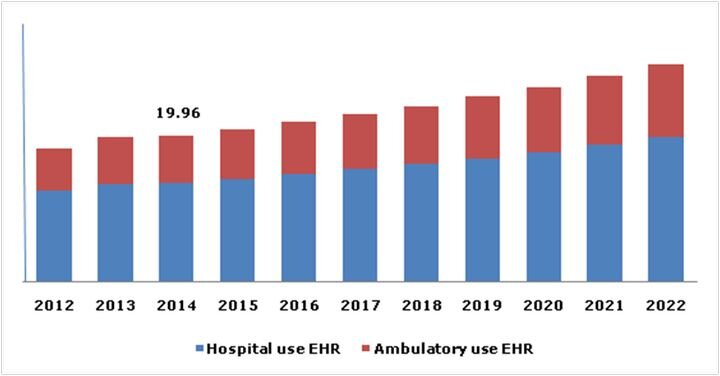
FELIXprinters has released a new bioprinter, the FELIX BIOprinter, which is quite a change for the long-time 3D printer manufacturer.